Distal Femur Fracture

A fracture is a broken bone. Fractures of the thighbone that occur just above the knee joint are called distal femur fractures. The distal femur is where the bone flares out like an upside-down funnel.
Distal femur fractures most often occur either in older people whose bones are weak, or in younger people who have high energy injuries, such as from a car crash. In both the elderly and the young, the breaks may extend into the knee joint and may shatter the bone into many pieces.
Distal femur fractures vary. The bone can break straight across (transverse fracture) or into many pieces (comminuted fracture). Sometimes these fractures extend into the knee joint and separate the surface of the bone into a few (or many) parts. These types of fractures are called intra-articular. Because they damage the cartilage surface of the bone, intra-articular fractures can be more difficult to treat.
Distal femur fractures can be closed — meaning the skin is intact — or can be open. An open fracture is when a bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the broken bone. Open fractures often involve much more damage to the surrounding muscles, tendons, and ligaments. They have a higher risk for complications and take a longer time to heal.
When the distal femur breaks, both the hamstrings and quadriceps muscles tend to contract and shorten. When this happens the bone fragments change position and become difficult to line up with a cast.
DISTAL FEMUR ANATOMY

DISEASE EXPLAINED

SYMPTOMS
The most common symptoms of distal femur fracture include:
Pain with weightbearing
Swelling and bruising
Tenderness to touch
Deformity — the knee may look “out of place” and the leg may appear shorter and crooked
In most cases, these symptoms occur around the knee, but you may also have symptoms in the thigh area.
CAUSES
Fractures of the distal femur most commonly occur in two patient types: younger people (under age 50) and the elderly.
Distal femur fractures in younger patients are usually caused by high energy injuries, such as falls from significant heights or motor vehicle collisions. Because of the forceful nature of these fractures, many patients also have other injuries, often of the head, chest, abdomen, pelvis, spine, and other limbs.
Elderly people with distal femur fractures typically have poor bone quality. As we age, our bones get thinner. Bones can become very weak and fragile. A lower-force event, such as a fall from standing, can cause a distal femur fracture in an older person who has weak bones. Although these patients do not often have other injuries, they may have concerning medical problems, such as conditions of the heart, lungs, and kidneys, and diabetes.
TREATMENT
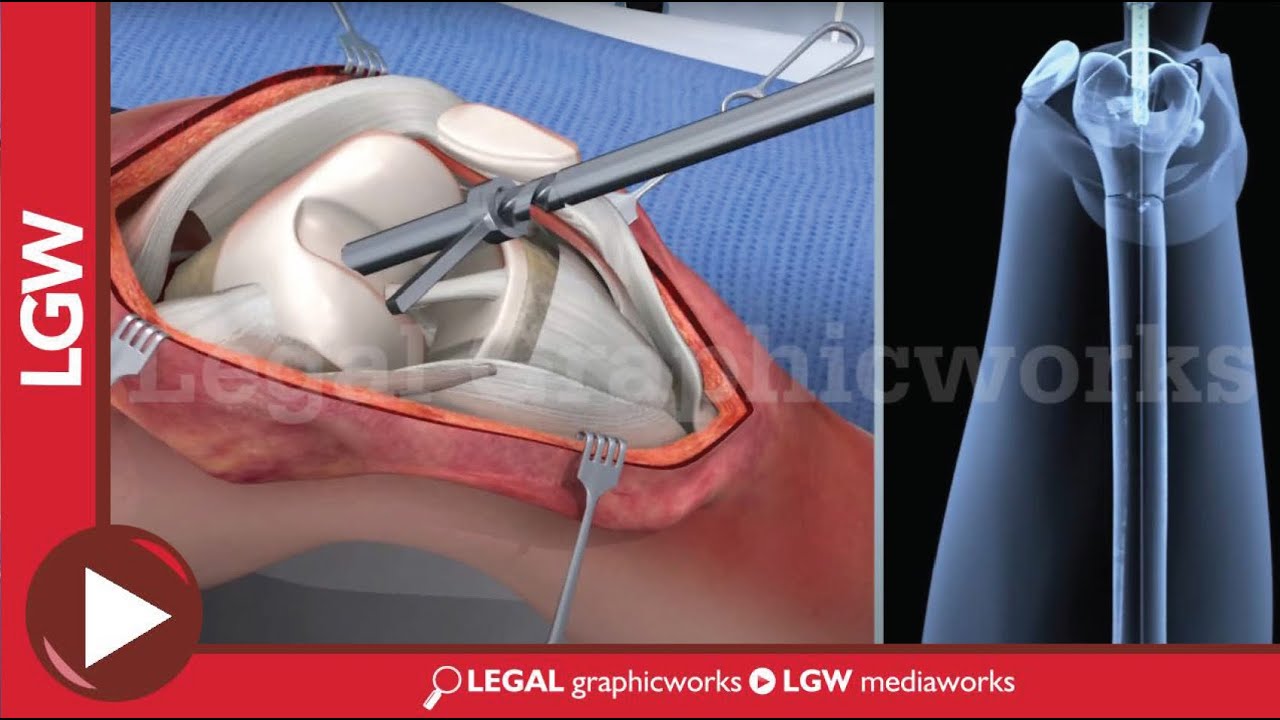
TREATMENT OPTIONS
NONSURGICAL TREATMENT
Nonsurgical treatment options for distal femur fractures include:
SKELETAL TRACTION.
Skeletal traction is a pulley system of weights and counterweights that holds the broken pieces of bone together. A pin is placed in a bone to position the leg.
CASTING AND BRACING.
Casts and braces hold the bones in place while they heal. In many cases of distal femur fracture, however, a cast or brace cannot correctly line up the bone pieces because shortened muscles pull the pieces out of place. Only fractures that are limited to two parts and are stable and well aligned can be treated with a brace. Casts and braces can also be uncomfortable.
Patients with distal femoral fractures of all ages do best when they can be up and moving soon after treatment (such as moving from a bed to a chair, and walking). Treatment that allows early motion of the knee lessens the risk of knee stiffness, and prevents problems caused by extended bed rest, such as bed sores and blood clots.
Because traction, casting, and bracing do not allow for early knee movement, they are used less often than surgical treatments. Your doctor will talk with you about the best treatment option for you and your injury.
SURGICAL OPTIONS
Because of newer techniques and special materials, the results of surgical treatment are good, even in older patients who have poor bone quality.
TIMING OF SURGERY.
Most distal femur fractures are not operated on right away — unless the skin around the fracture has been broken (open fracture). Open fractures expose the fracture site to the environment. They urgently need to be cleansed and require immediate surgery.
In most cases, surgery is delayed 1 to 3 days to develop a treatment plan and to prepare the patient for surgery. Depending on your age and medical history, your surgeon may recommend that you are evaluated by your primary doctor to make sure that you have no medical problems that need to be addressed before surgery.
EXTERNAL FIXATION.
If the soft tissues (skin and muscle) around your fracture are badly damaged, or if it will take time before you can tolerate a longer surgery because of health reasons, your doctor may apply a temporary external fixator. In this type of operation, metal pins or screws are placed into the middle of the femur and tibia (shinbone). The pins and screws are attached to a bar outside the skin. This device is a stabilizing frame that holds the bones in the proper position until you are ready for surgery.
When you are ready, your surgeon will remove the external fixator and place internal fixation devices on or in the bone under the skin and muscles.
INTERNAL FIXATION.
The internal fixation methods most surgeons use for distal femur fractures include:
INTRAMEDULLARY NAILING.
During this procedure, a specially designed metal rod is inserted into the marrow canal of the femur. The rod passes across the fracture to keep it in position.
PLATES AND SCREWS.
During this operation, the bone fragments are first repositioned (reduced) into their normal alignment. They are held together with special screws and metal plates attached to the outer surface of the bone.
Both of these methods can be done through one large incision or several smaller ones, depending on the type of fracture you have and the device your surgeon uses.
If the fracture is in many small pieces above your knee joint, your surgeon will not try to piece the bone back together like a puzzle. Instead, your surgeon will fix a plate or rod at both ends of the fracture without touching the many small pieces. This will keep the overall shape and length of the bone correct while it heals. The individual pieces will then fill in with new bone, called a callous.
In cases where a fracture may be slow to heal, such as when a patient is elderly with poor bone quality, a bone graft may be used to help the callous develop. Bone grafts may be obtained from the patient (most often taken from the pelvis) or from a tissue bank (cadaver bone). Other options include the use of artificial bone fillers.
In extreme cases, a fracture may be too complicated and the bone quality too poor to fix. These types of fractures are often treated by removing the fragments and replacing the bone with a knee replacement implant.
FRACTURES AND KNEE REPLACEMENTS.
As the population ages and the number of knee replacements rises, an increasing problem has emerged: More distal femur fractures are being seen in seniors who have knee replacements.
Those fractures are typically treated with rods or plates, just like other distal femur fractures. In rare cases, the artificial implant must be removed and replaced with a larger implant. This procedure is called a revision and may be necessary if the implant is loose or not supported by surrounding good bone.
DISCLAIMER
- All of the opinions expressed within the educational information delivered within the provided links are those of their authors and not necessarily those of either your treating doctor or CRO.
- This site is for educational purposes only!!
- Copyright Disclaimer under Section 107 of the copyright act 1976, allowance is made for fair use for purposes such as criticism, comment, news reporting, scholarship, and research. Fair use is a use permitted by copyright statutes that might otherwise be infringing. Non-profit, educational, or personal use tips the balance in favor of fair use.
